- 14-1-3/1, Nowroji Rd, Opp More Supermarket, Visakhapatnam
- spineleela@gmail.com
- +91 95739 17693
Spinal Implants—Frequently Asked Questions
Home > Blog > Spinal Implants—Frequently Asked Questions
Spinal Implants
🔹 What are spinal implants?
Spinal implants are medical devices placed inside the body during spine surgery.
🔹 What types of spinal implants are commonly used?
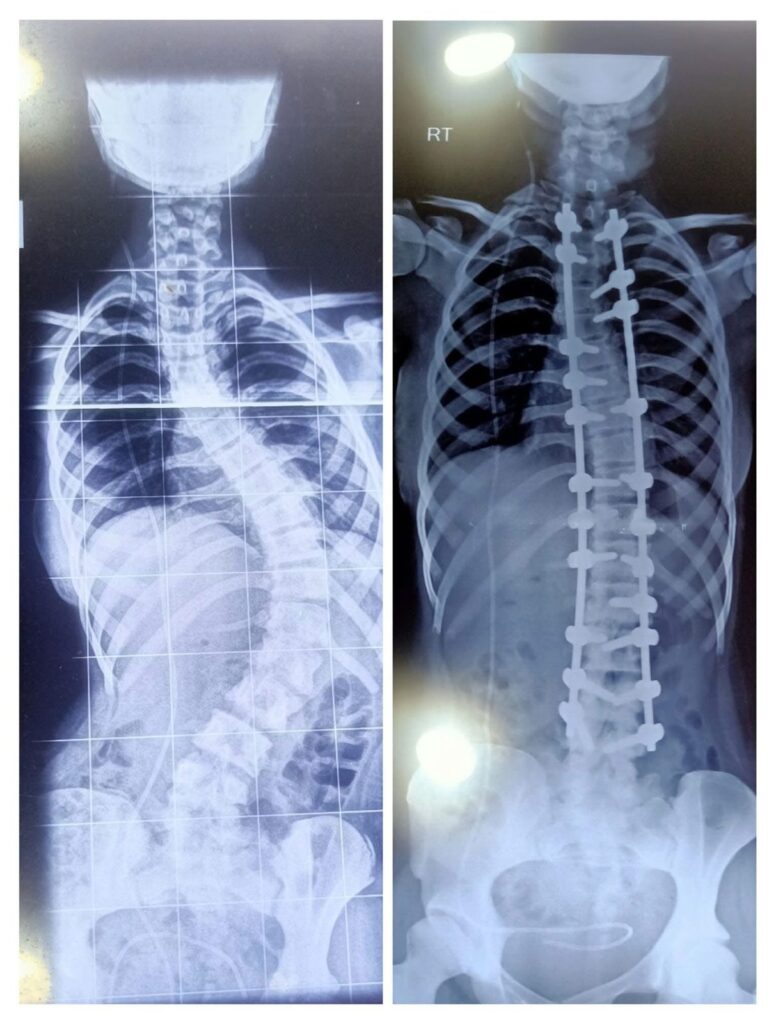
Pedicle screws, hooks, and rods: Used to stabilize the spine and hold the bones in proper alignment.

Plates: Commonly used in the cervical spine (neck) to support stability and protect the bone graft.

Interbody cages: Placed between vertebrae to maintain disc height and promote bone fusion.

Artificial discs: Used to replace damaged spinal discs while preserving spinal motion.
Wires and connectors: Sometimes used to provide additional support in complex spinal surgeries.
The type of implant used depends on:
- The patient’s spinal condition
- Age
- Bone quality
- Surgical goals
🔹 What materials are spinal implants made of?
Most spinal implants are made from:
- Titanium
- Cobalt-chromium alloys
- Medical-grade plastics (eg, PEEK)
- Stainless steel
These materials are safe, biocompatible, and well-tested for use in the human body.
🔹 What are the indications for spinal implants?
Spinal implants are used to stabilize, support, or correct the spine in conditions such as:
- Spinal instability causing pain and functional impairment (spondylolysis, spondylolisthesis)
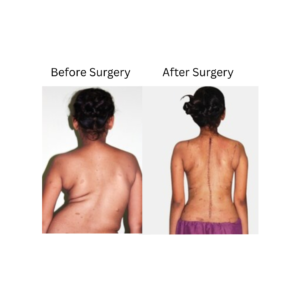
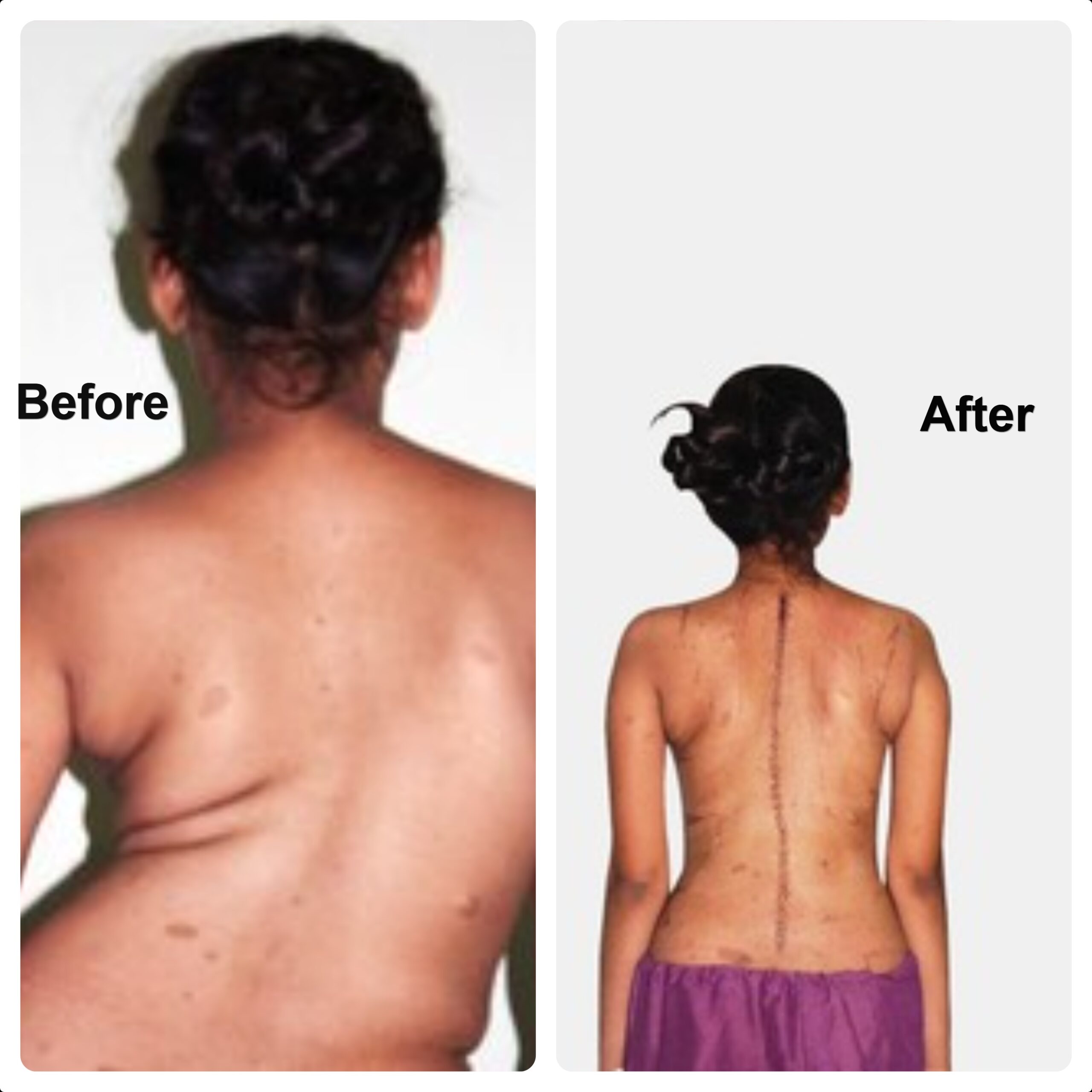
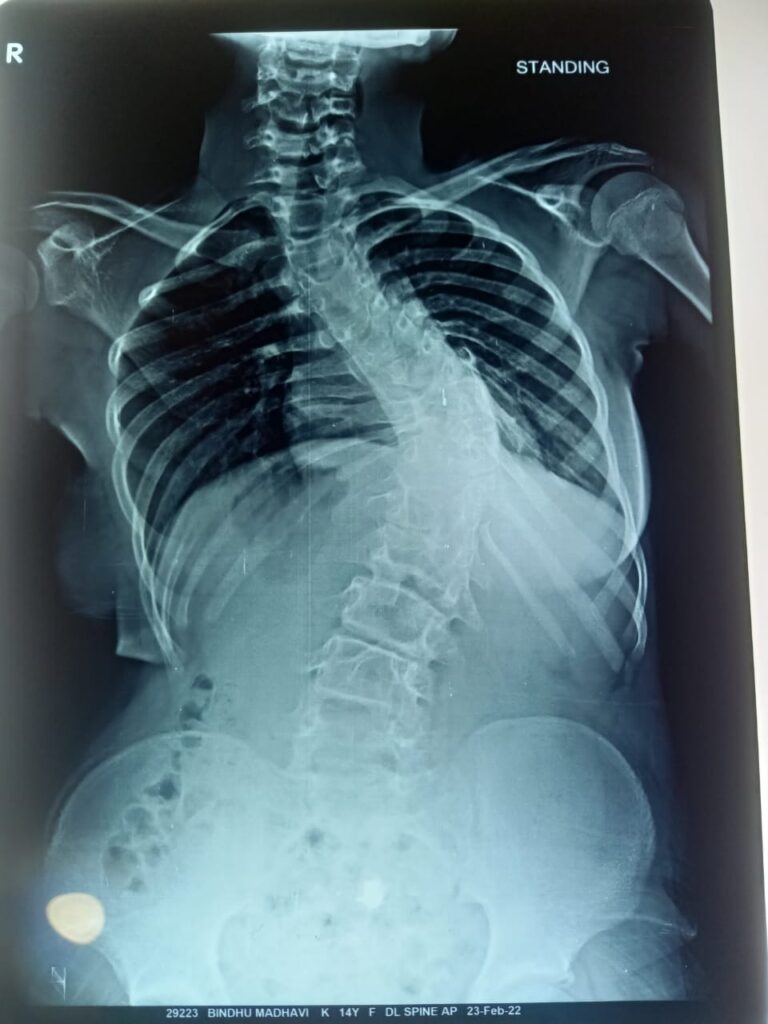
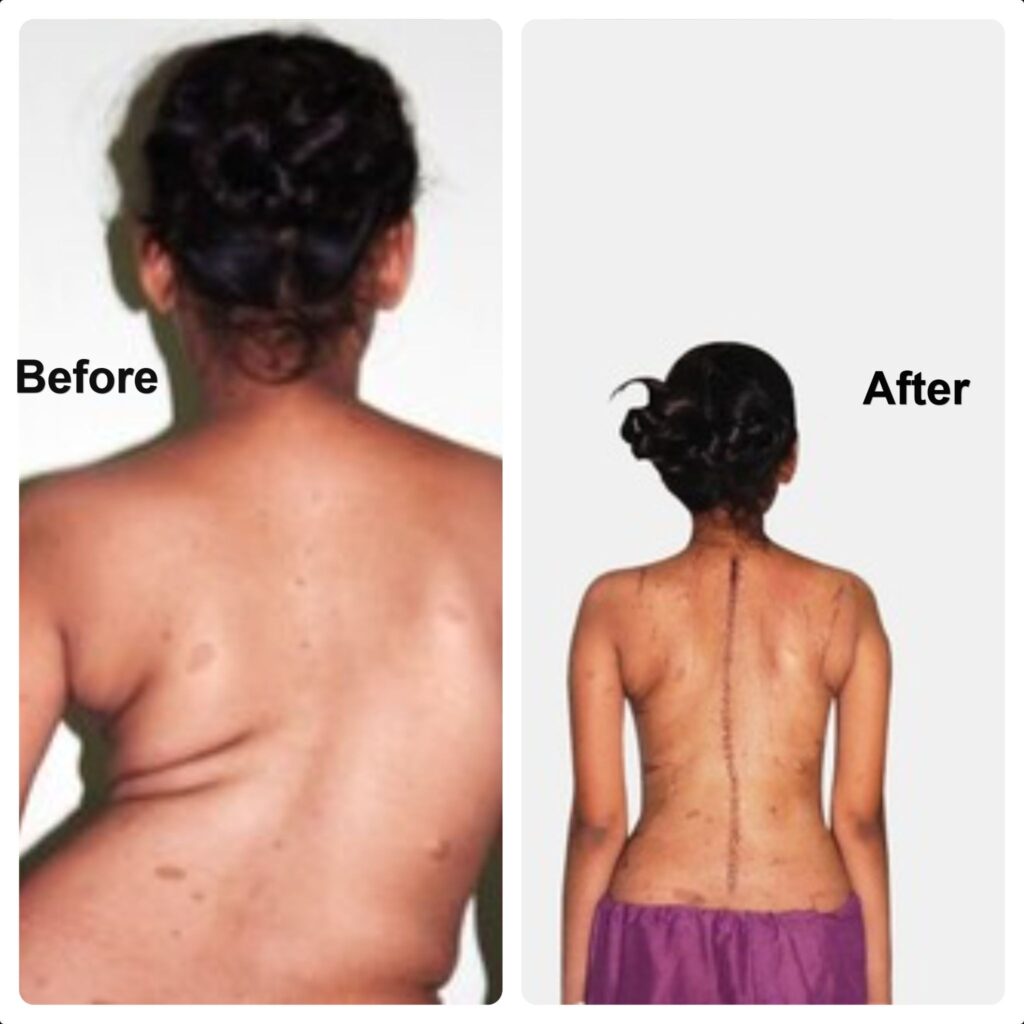
- Spinal deformities (scoliosis, kyphosis) — to correct deformity and maintain spinal alignment
- Spine fractures and dislocations — to restore alignment, stabilize the spine, relieve pain, and allow early mobilization
- Spinal tumors and infections — to stabilize and reconstruct the spine
- Failed previous spine surgery (revision surgery)
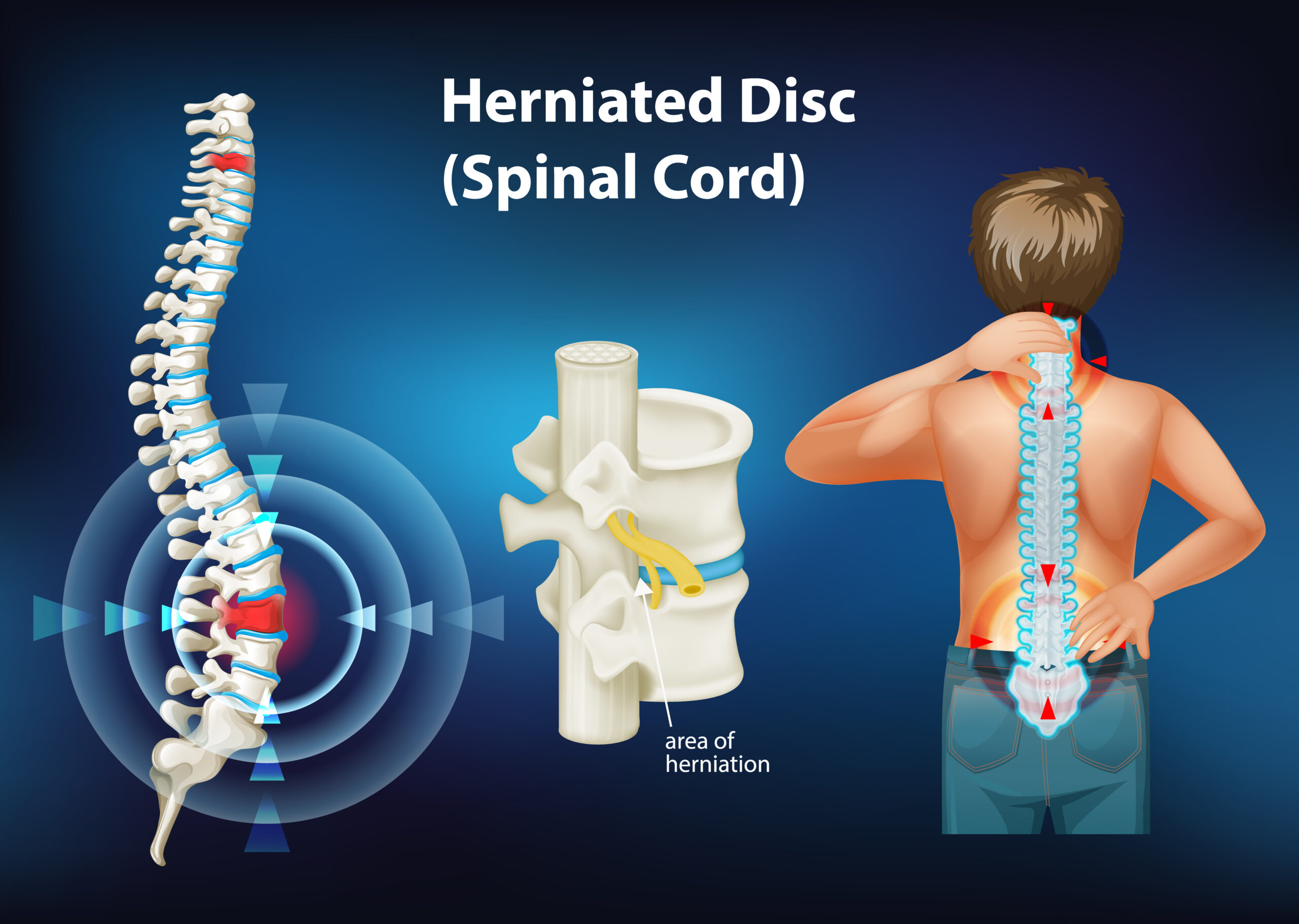
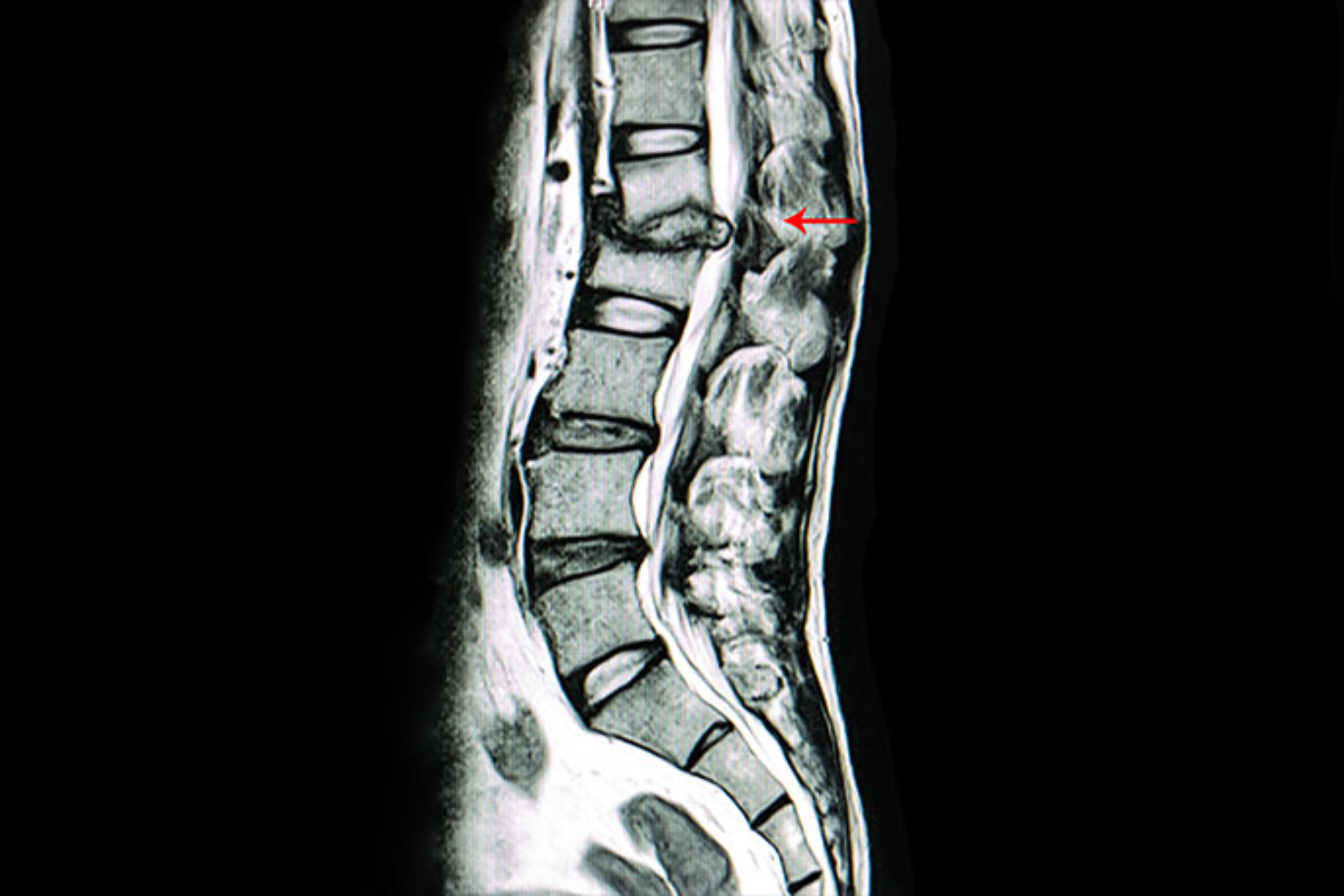
- Slipped disc and spinal canal stenosis when significant bone removal is required for adequate decompression
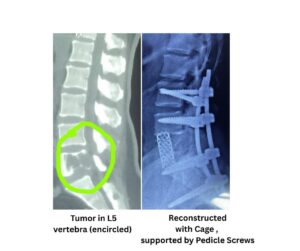
🔹 Do spinal implants help in bone healing?
Yes. Many spinal implants are designed to facilitate bone healing by providing stability, especially after spinal fusion surgery. However, implants themselves do not directly heal bone.
During spinal fusion surgery, a bone graft is placed along with the implants. The implants keep the spine stable while the bone graft gradually grows and fuses adjacent vertebrae into one solid bone over several months.
🔹 Are spinal implants safe?
Yes. Spinal implants are generally very safe, and complications are uncommon.
Possible complications include:
- Infection
- Implant loosening or breakage
- Malpositioning of implants
- allergic reactions( very rare)
Usually, surgeons take several precautions to minimize these risks.
🔹 What is malpositioning of spinal implants?
Malpositioning means that a screw, rod, cage, or other implant is not placed in the ideal position during surgery.
Depending on the severity and location, possible complications include:
- Persistent back or neck pain
- Nerve injury causing pain, numbness, tingling, or weakness
- Spinal cord injury (rare but serious)
- Implant loosening or failure
- Poor bone fusion (non-union)
- Reduced deformity correction
- Damage to nearby blood vessels, lungs, or internal organs
- Need for revision surgery
Precise surgical techniques and modern technologies improve implant accuracy and reduce complications.
🔹 Can I walk and do normal activities after surgery?
Yes. Most patients are encouraged to start walking within a day or two after surgery, and daily activities are gradually resumed over weeks to months, depending on the procedure and overall condition.
However, during early recovery, patients are usually advised to avoid heavy lifting, excessive bending/twisting and high-impact activities
🔹 Will spinal implants remain in the body forever, or do they need to be removed?
In most cases, spinal implants are designed to remain in the body permanently. They are made from biocompatible materials and usually do not need removal once the bone has healed and the spine is stable.
Implant removal is uncommon and may be considered if the patient develops:
- Infection
- Implant loosening or breakage
- Persistent pain or irritation
- Rare allergic reactions
Important exception:
When implants are used temporarily to stabilize lumbar spine fractures, especially in younger patients, surgeons may sometimes remove them 1–2 years after the fracture has healed. It may help restore lower back movement and flexibility.
Overall, most patients live their entire lives with spinal implants without problems.
🔹 Will I feel the implant inside my body?
Usually not. Most patients do not feel the implant once healing is complete.
🔹 Will spinal implants trigger metal detectors?
Usually not. Most spinal implants do not trigger airport security alarms.
🔹 Can patients undergo MRI scans after spinal implant surgery?
Yes. Most modern implants, especially titanium implants, are MRI-compatible and safe for MRI scans.
🔹 Can spinal implants fail or break?
Yes. Although modern spinal implants are very durable, breakage can occur, especially if healing does not occur properly.
Common causes of implant failure include:
- Failure of bone fusion (pseudarthrosis)
- Excessive mechanical stress
- Poor bone quality (such as osteoporosis)
- Infection
- Long spinal constructs
- Implant fatigue over time
- Improper spinal alignment or surgical factors
🔹 Do spinal implants cure back pain completely?
Not always. Spinal implants can stabilize the spine, reduce pain caused by instability and improve quality of life.
However, some patients may continue to have mild discomfort even after successful surgery.
🔹 Is spine surgery with implants very risky?
Spine surgery is a major procedure, but modern surgical techniques have made it much safer than before.
Most patients achieve good outcomes when they have surgery for the right reasons and follow it with proper rehabilitation.
🔹 Can I live a normal life after spinal implant surgery?
Yes, most patients return to normal daily activities. resume work, travel, and participate in exercise and recreational activities
Many people lead active and healthy lives after recovery from spinal implant surgery.
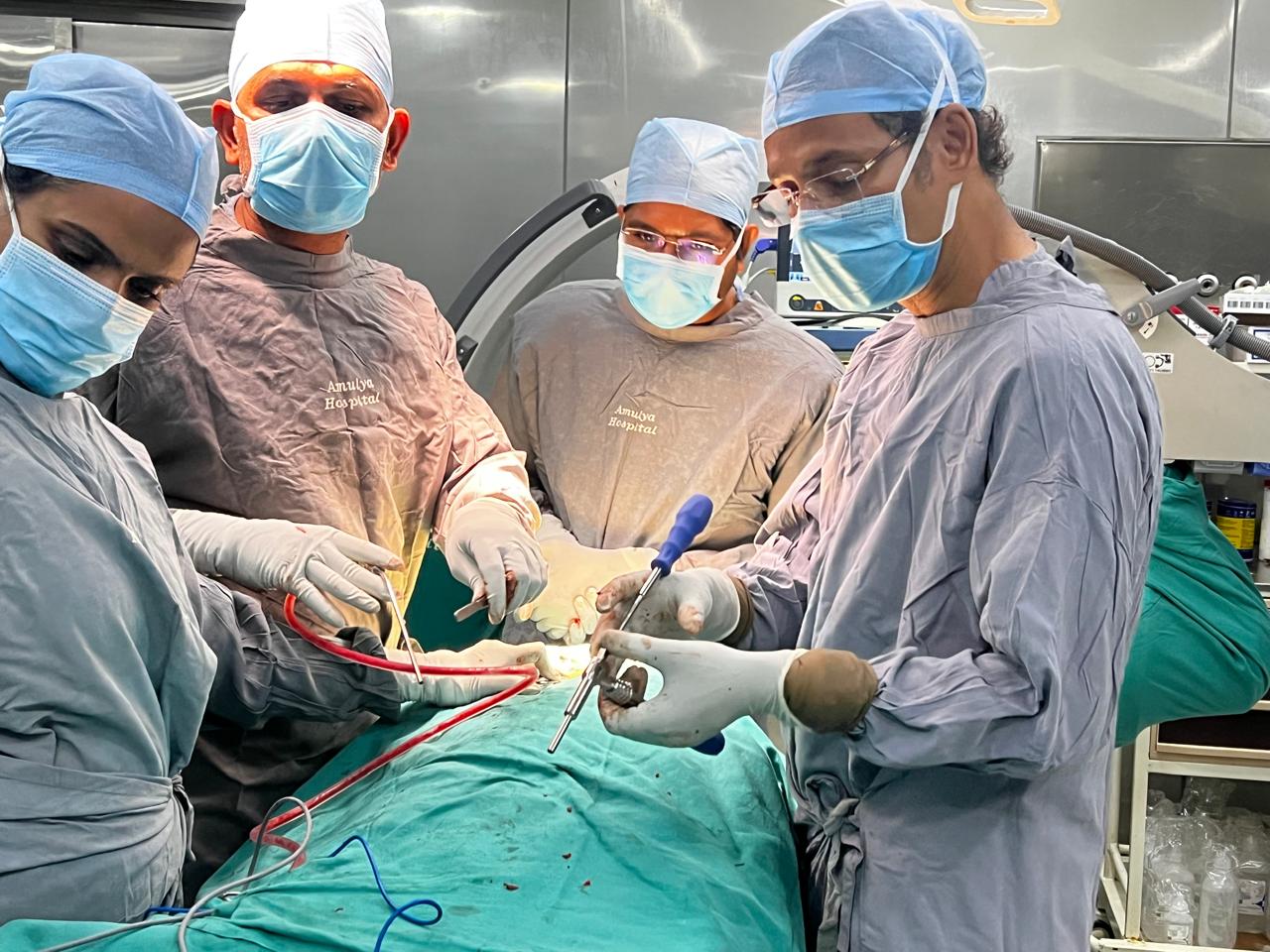
Spinal Implant—Dr. B. Leela Prasad Spine Specialist
Dr. B. Leela Prasad at Amulya Hospital specializes in spine surgery in Visakhapatnam and provides advanced surgical and nonsurgical treatment for patients suffering from spine disorders, fractures, disc problems, and spinal instability. With expert care, modern surgical techniques, and personalized recovery support, patients receive effective treatment for long-term spine health and improved mobility.
Dr. B Leela Prasad

Dr. B. Leela Prasad is one of the country’s most renowned orthopedic doctors, with over 15 years of experience in the field. After earning his medical degree from Andhra Medical College, Visakhapatnam, he pursued post-graduation in Orthopedics at Guntur Medical College.
Visit Us at
- Amulya Hospital
- 14-1-3/1, Nowroji Rd, Opp More Supermarket, Visakhapatnam
- spineleela@gmail.com
- +91 95739 17693
- Hyma Nursing Home
- Main Road, Marripalem, Visakhapatnam-18
- HYMA Nursing : 07:30PM – 09:30 PM


 Key Message:
Key Message:
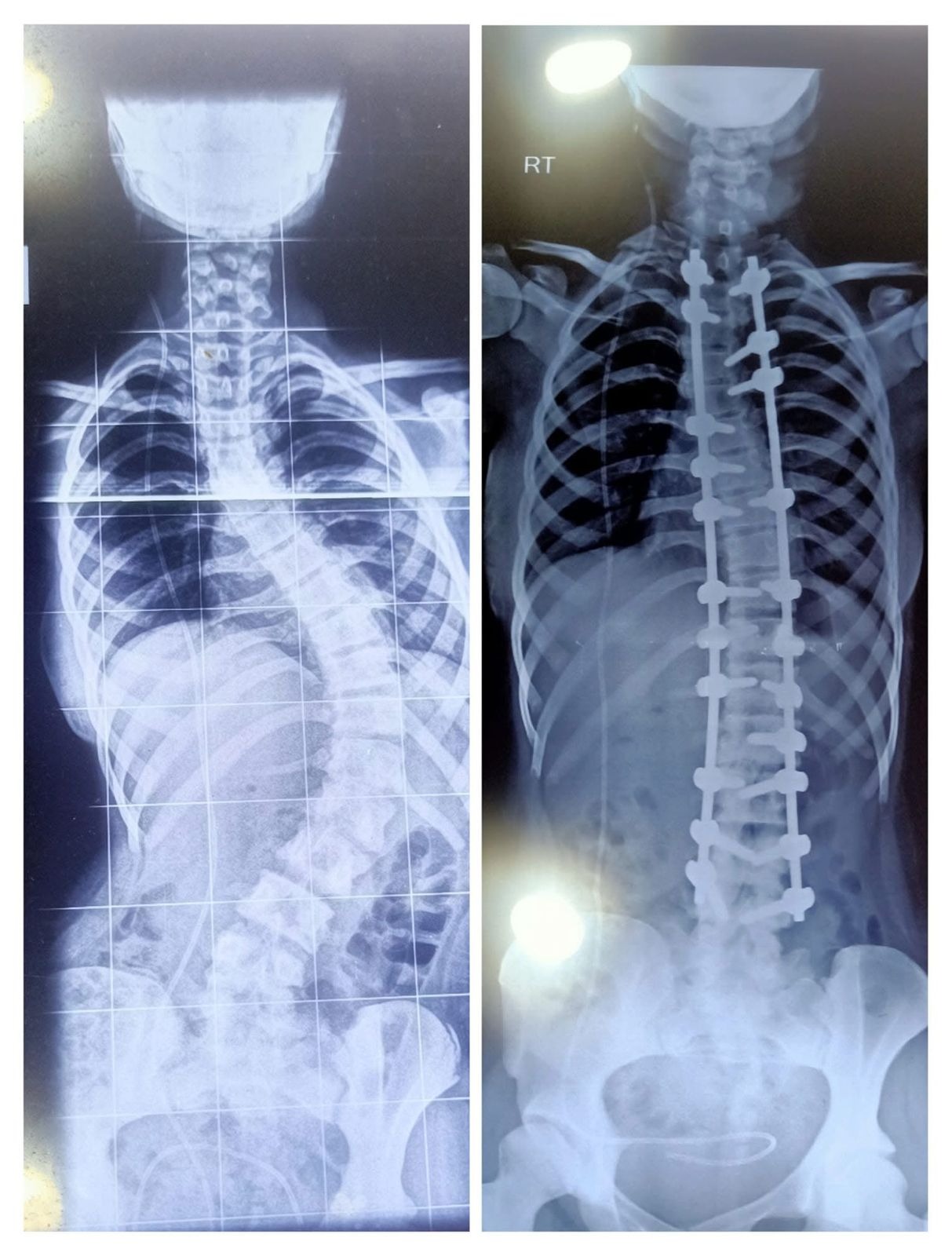
 Myth 1: “Carrying heavy school bags/backpacks causes scoliosis.”
Myth 1: “Carrying heavy school bags/backpacks causes scoliosis.”