Common Myths About Back Pain
Common Myths About Back Pain 1. Myth: Back pain always means there is a serious spine problem. Fact:Most episodes of back pain are due to muscle strain, poor posture, or unaccustomed activity. They usually improve with rest, physiotherapy, and simple medication. Only a small percentage of cases are caused by serious conditions such as infection, […]
10 FAQs regarding TB Spine
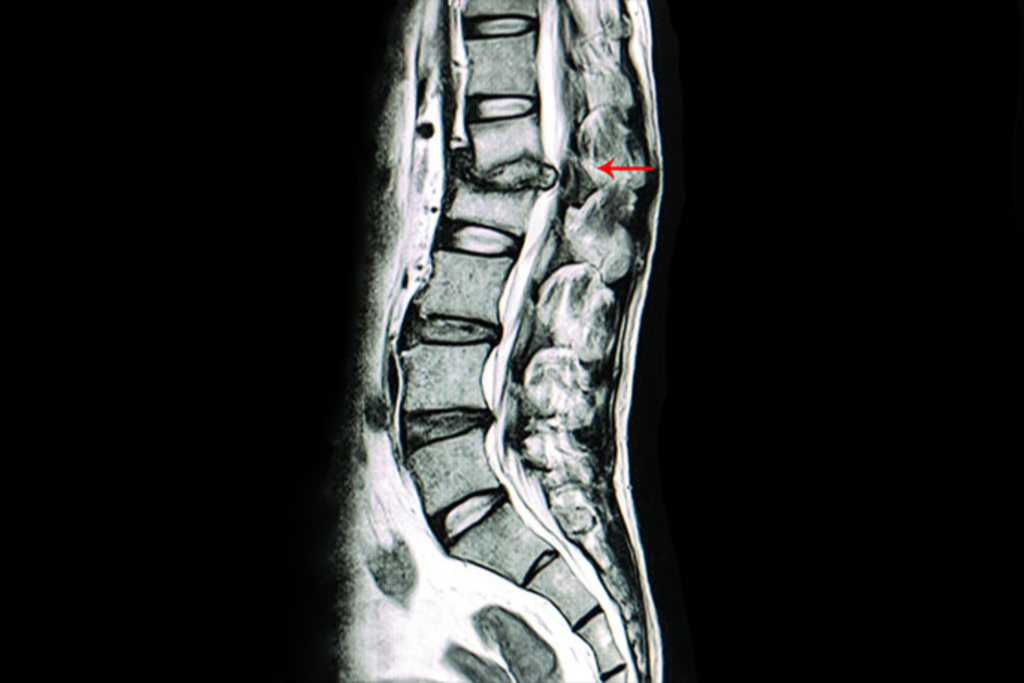
Q1. Many people think TB affects only the lungs. Does it really affect the spine? Though TB commonly affects the lungs, it can also affect bones and joints (called skeletal tuberculosis).In fact, the spine is the most common site of bone TB. Get the best tuberculosis spine treatment in Vizag from Dr. B. Leela Prasad. […]