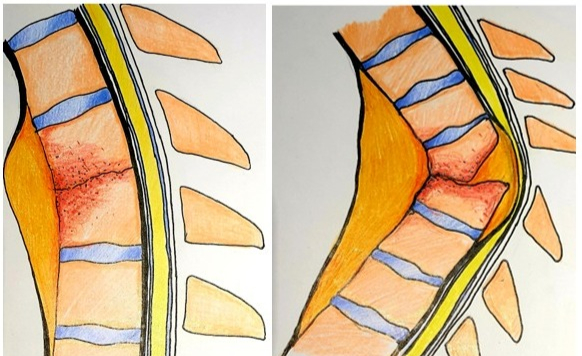
Scoliosis is a structural disorder in which the spine bends sideways instead of being straight. While the spine typically exhibits gentle front-to-back curves that help maintain balance and absorb shock, scoliosis involves a side-to-side bending accompanied in many cases by vertebral rotation. This condition is most often noticed in children or teenagers, especially during periods of rapid growth, though it can affect people of any age.
Types and causes
- Adolescent idiopathic scoliosis: It is the most common type of scoliosis, accounting for nearly 80% of all cases. It develops during adolescence and has no clearly identifiable cause. The condition is more frequently seen in girls. Although its exact cause remains unknown, a combination of genetic, hormonal, and neuromuscular factors is thought to play a role, with no single mechanism definitively established.
- Congenital scoliosis: It results from abnormalities in vertebral development during fetal growth, such as fused, missing, or incompletely formed vertebrae.
- Neuromuscular scoliosis: It arises secondary to conditions such as cerebral palsy, muscular dystrophy, or spinal cord injury, in which weakened or imbalanced muscles are unable to provide adequate support to the spine.
- Degenerative scoliosis: It develops in older adults as a result of age-related wear and tear of the intervertebral discs and facet joints, leading to progressive spinal curvature.
Symptoms
Symptoms of scoliosis vary from mild to severe depending on the extent of spinal curvature. In mild cases, the condition may remain unnoticed and is often detected only during routine screening. Common visible signs include uneven shoulders, a tilted waistline, one hip appearing higher than the other, or a noticeable rib hump when bending forward. Scoliosis usually does not cause pain in children and adolescents; however, adults may experience back pain, muscle fatigue, and stiffness. In severe cases, significant spinal curvature can reduce chest cavity space, potentially leading to breathing difficulties and, in rare instances, impaired heart function due to restricted organ capacity.
Diagnosis & Imaging tests
Scoliosis is typically diagnosed through a physical examination. The spinal curvature becomes more apparent when the patient is asked to bend forward, a manoeuvre known as the forward bend test. X-rays are used to confirm the diagnosis and to measure the severity of the curvature using the Cobb angle. Curves less than 20 degrees are generally classified as mild, those between 20 and 40 degrees as moderate, and curves greater than 40–50 degrees as severe.
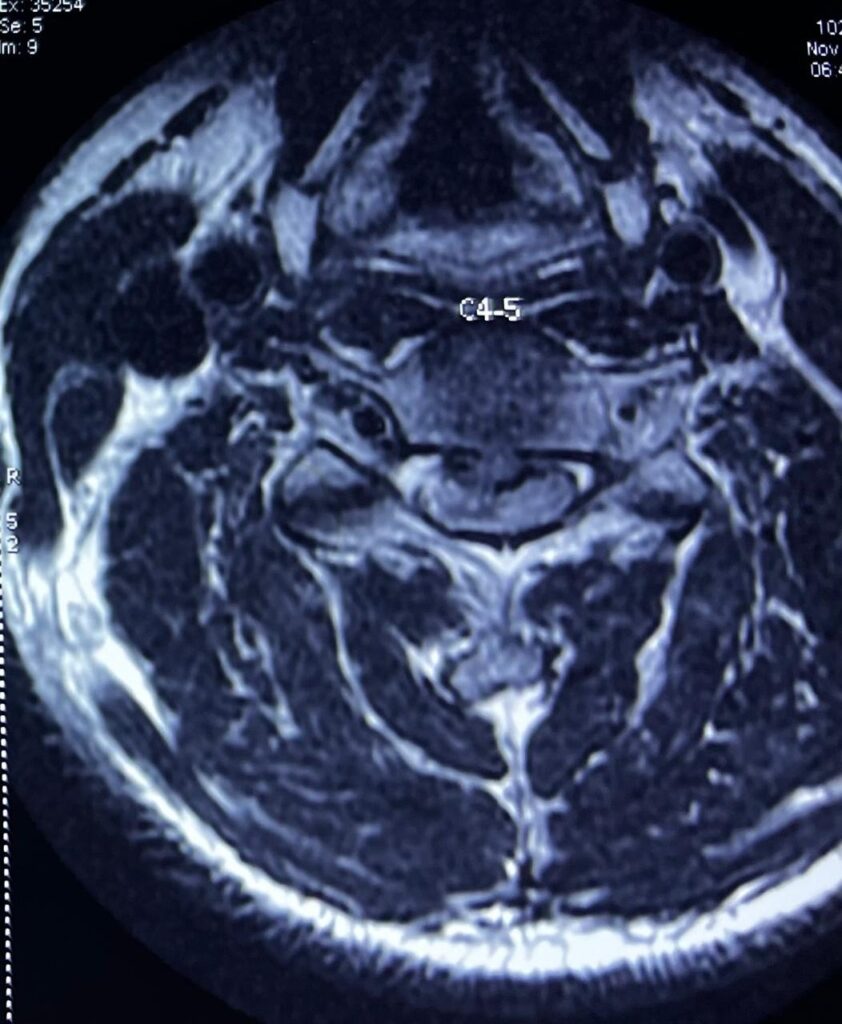
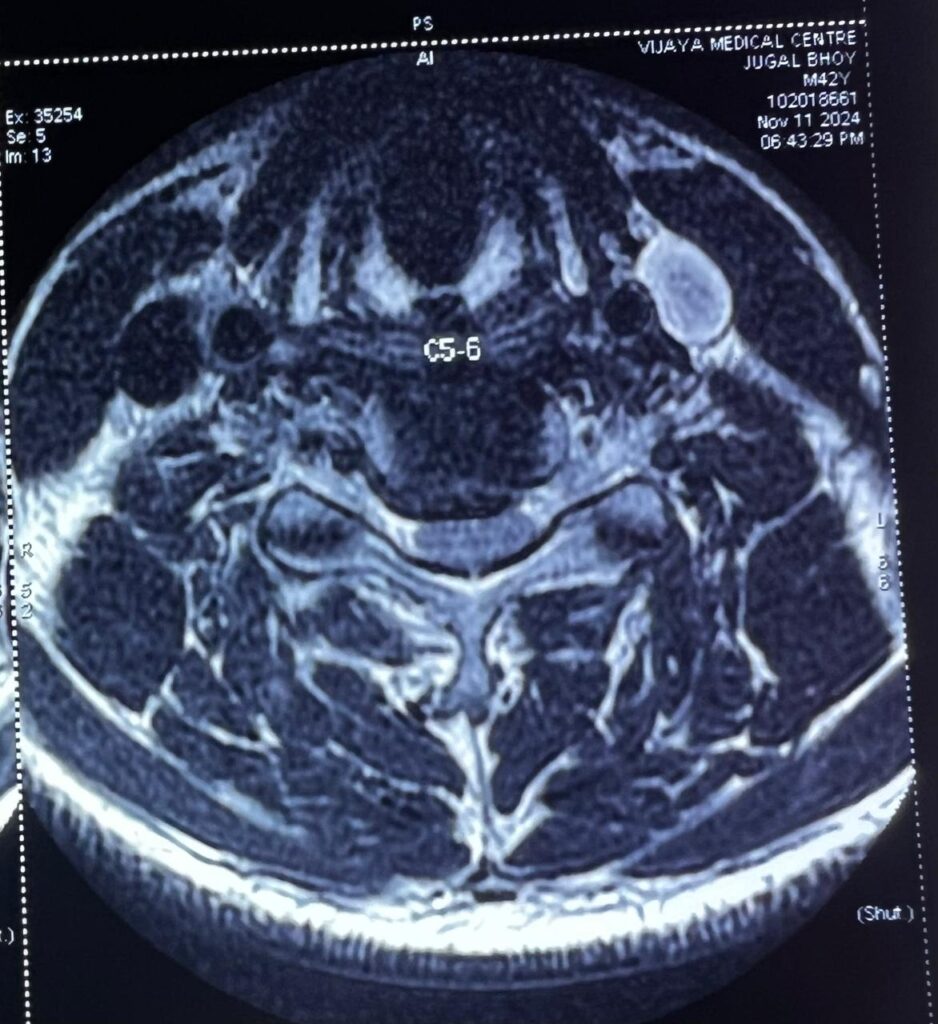
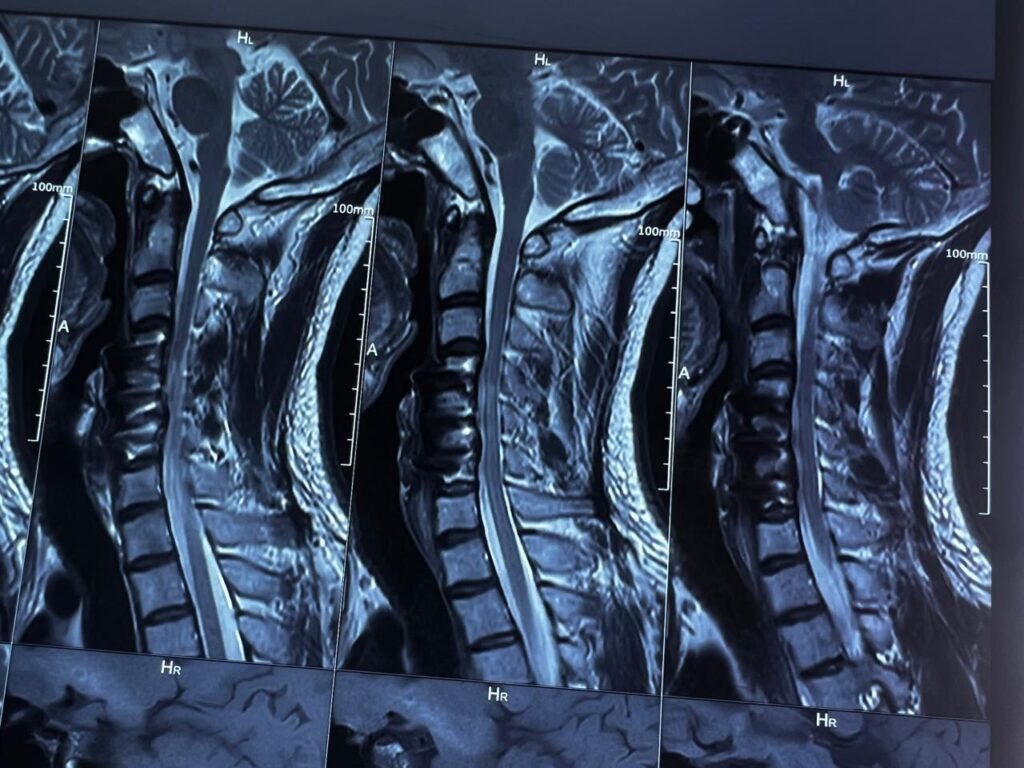
MRI scans may be performed to rule out underlying abnormalities of the spinal cord.
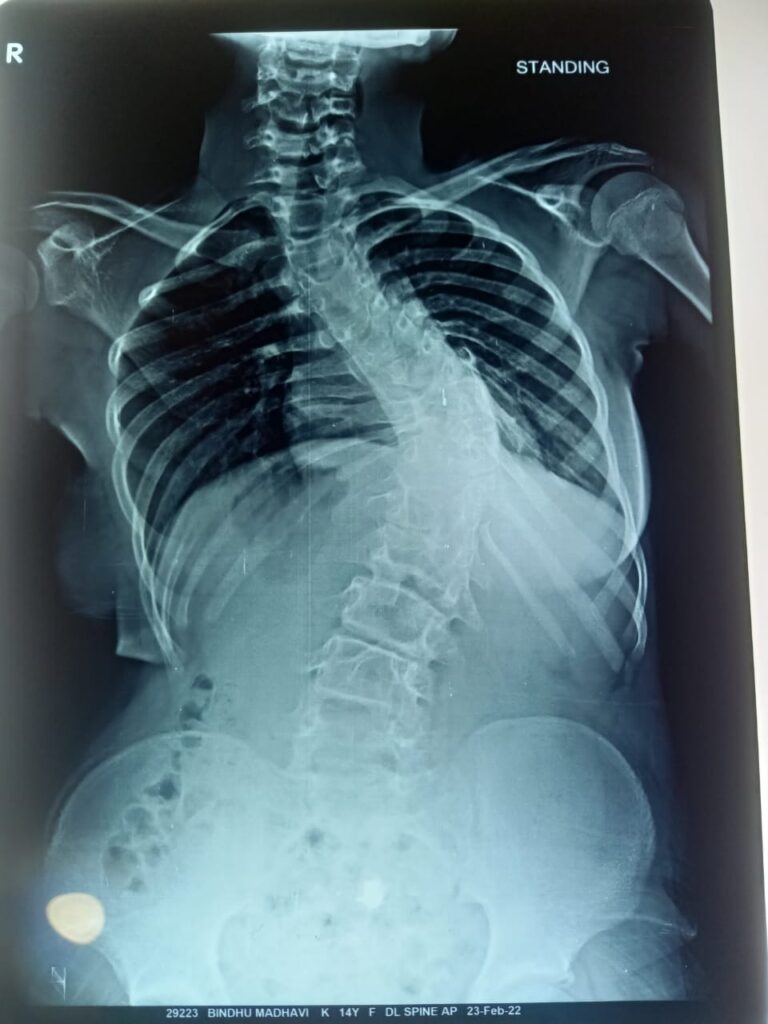
Scoliosis Treatment – MRI scans
Follow-up and Risk of Progression:
Growing children require regular follow-up, typically with X-rays every six months, to monitor changes in the spinal curvature. The risk of curve progression depends on several factors, including the child’s age, remaining growth potential, and the magnitude of the curve at the time of diagnosis.
Treatment:
Scoliosis treatment depends on the spinal curve size and the child’s expected growth. Even children with slight curves require regular follow-up to monitor whether the curvature worsens during growth—older adolescents who have stopped growing and have mild curves often do not need active treatment. Overall, management is individualised based on the patient’s age, curve severity, and risk of progression.
Bracing:
It is a key treatment option for moderate scoliosis, particularly in adolescents who are still growing. While braces do not correct or straighten the spine, they are effective in preventing further progression of the curve. For optimal effectiveness, the brace must be worn for about 20 hours per day and is usually worn under clothing. The success of bracing increases with the number of hours it is worn. Children wearing braces can continue to participate in most daily activities, and once growth is complete, bracing may no longer be necessary.
Surgical correction:
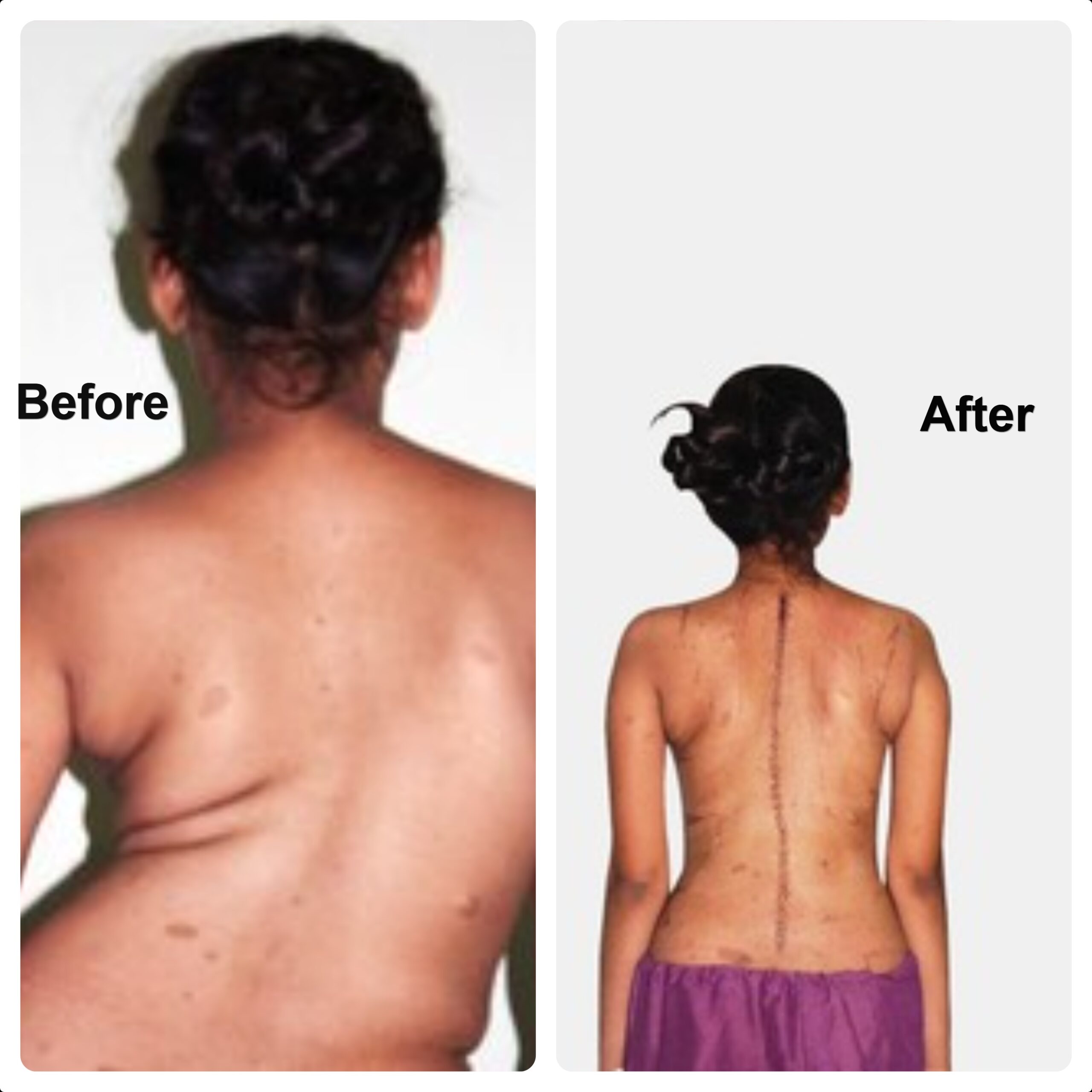
It is generally recommended for severe curves (Cobb angle greater than 50 degrees) or for deformities that are likely to progress despite conservative management. Surgery typically involves placing titanium screws into the vertebrae, connecting them with rods, and correcting the deformity through controlled manoeuvres. Bone grafts are then placed to achieve spinal fusion, which helps stabilise the spine and prevent further progression of the curve.
Scoliosis—Before and After Surgery
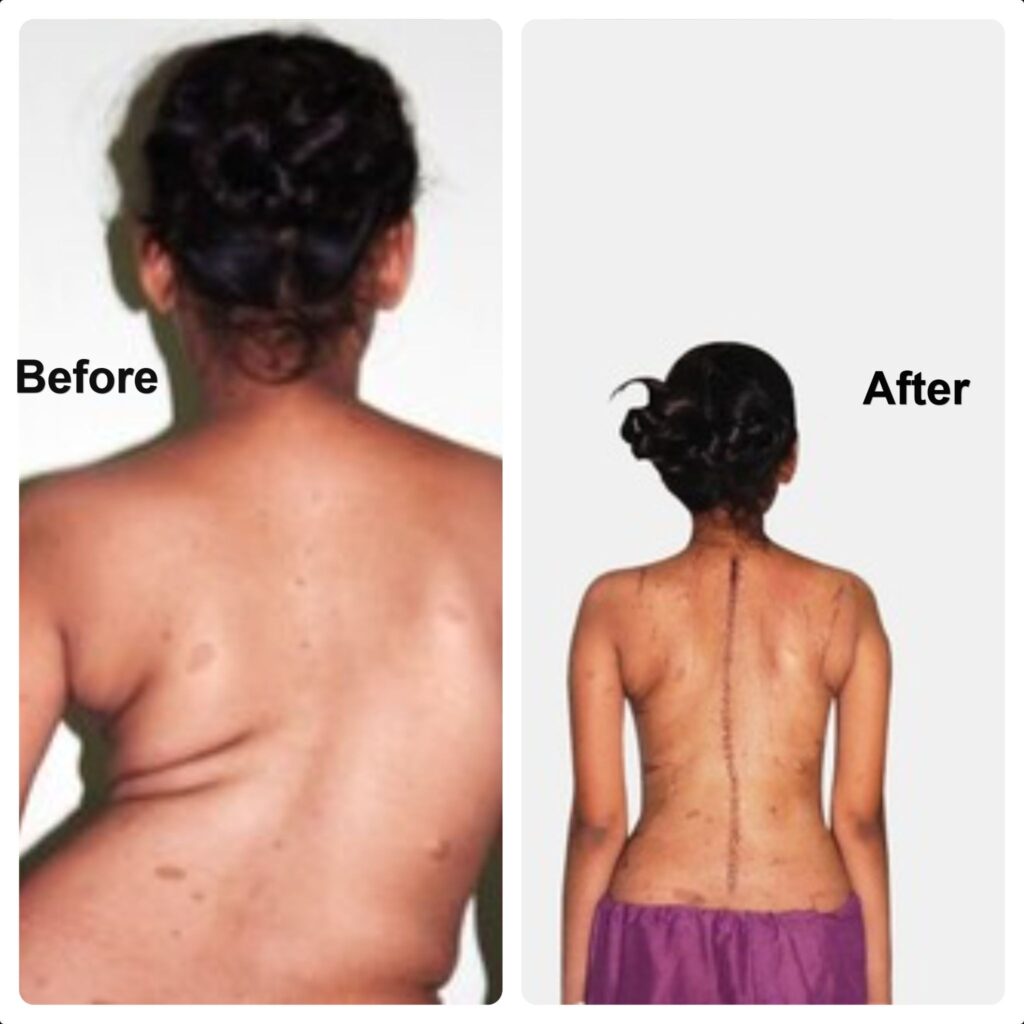
Complications of scoliosis surgery:
Scoliosis correction is a major surgical procedure that carries the risk of several potential complications. These include significant blood loss, infection, weakness of the legs or paralysis due to injury to the spinal cord, complications related to anaesthesia, the possible need for postoperative ICU care, and problems associated with the surgical implants used for spinal stabilisation. Rarely, the spine may continue to curve above or below the surgically corrected segment, leading to a progression of curvature adjacent to the surgery site.
Beyond medical treatments, lifestyle measures play an essential supportive role in the management of scoliosis. Physical therapy and regular exercise help improve muscle balance, posture, and core strength. Activities such as swimming, yoga, and Pilates can enhance flexibility, overall fitness, and comfort. Psychological support is equally essential, as adolescents with scoliosis may experience self-consciousness, stress, or anxiety related to body image and treatment.
Although once considered a dreaded condition, individuals with scoliosis can now lead active and productive lives. Patients can pursue normal daily activities, and women can safely bear children even after undergoing corrective surgery. With advances in medical expertise and surgical techniques, scoliosis surgery is no longer limited to major metropolitan centres, and effective treatment can be accessed in many well-equipped hospitals closer to home.
Scoliosis Treatment In Vizag-
Patients of all ages can get expert evaluation and personalised treatment plans from Dr B. Leela Prasad, who is known as the Best Spine Surgeon in Vizag for Scoliosis. He is known as a trusted Scoliosis Treatment Specialist in Visakhapatnam because he has years of experience treating complicated spine deformities. He uses cutting-edge technology along with caring support to make sure that patients get the proper treatment and long-lasting relief.
As an expert in Top Spine Surgeon Vizag Scoliosis Correction, Dr B. Leela Prasad uses both non-surgical and minimally invasive medical methods to treat scoliosis, depending on the needs of each patient. People in Vizag who want safe, effective, and long-lasting scoliosis treatment choose him. It is because he is dedicated to professional quality and patient-centred results.